The downfall of “idiopathic recurring stupor”
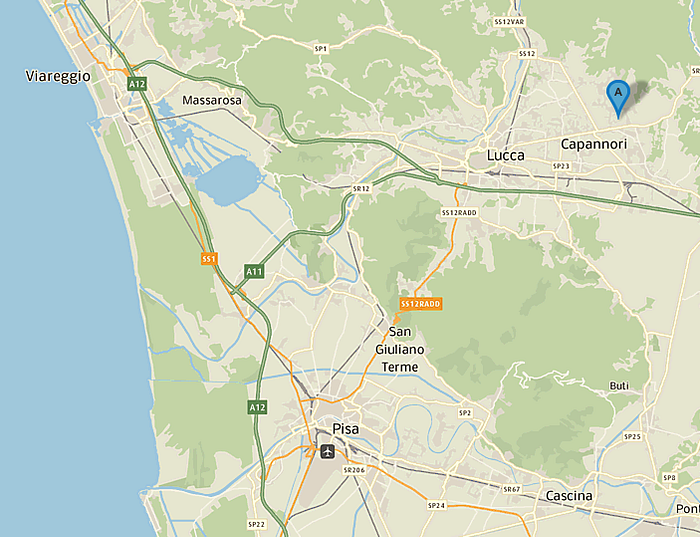
In the spring and summer of 1997, residents of Camigliano, a community in Tuscany near Lucca, began falling asleep under mysterious circumstances. One by one, seven people entered a trance-like lethargic state, typically lasting 10 to 20 hours. The strange somnolence affected a woman in her 80s more than 10 times, while affecting her neighbors and relatives between one and five times. The signs of onset were similar: dizziness, loss of coordination, sometimes nausea and then sleep. Some people could briefly respond to questions or even eat, but then returned to slumber. Upon waking, they did not remember what happened.
These individuals looked like they were under the influence of benzodiazepines, a class of drugs often prescribed for insomnia or anxiety. Some of the people displayed signs of benzodiazepine exposure when examined via EEG, and woke up when given the benzodiazepine antidote flumazenil. However, they swore that they hadn’t knowingly taken sleeping pills. The confusion set off a public health investigation and a wave of interest from media organizations. Elio Lugaresi, a distinguished sleep researcher from the University of Bologna, told reporters that the Camigliano incidents were examples of “idiopathic recurring stupor” (IRS), which he had published several papers on already. Lugaresi and his colleagues eventually discovered that they had made a mistake, and there was a simpler explanation.
I originally became interested in these incidents in connection with research on another sleep disorder: idiopathic hypersomnia, the shadow sibling of narcolepsy. Idiopathic hypersomnia (IH) describes people who experience a chronic increased need for sleep and excessive daytime sleepiness. People with IH have it all the time, not just occasionally.
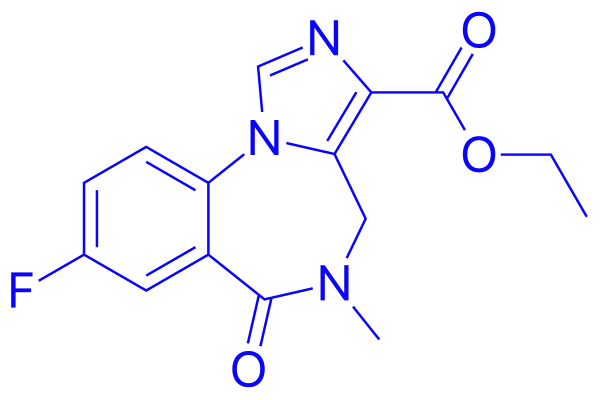
What connected IH and IRS, besides the word idiopathic, was the drug flumazenil, which has a weird many-branched history. David Rye and Lynn Marie Trotti, neurologists at Emory (where I work), have reported that some people with IH and related sleep disorders responded well to flumazenil — even though they weren’t taking benzodiazepines.
In my book The Woman Who Couldn’t Wake Up, I describe how this finding spurred people with IH to organize themselves and push for more attention to their condition. IH has been studied less than “classic” narcolepsy, but recently, European and American sleep specialists have been discussing how to redraw the diagnostic boundaries between narcolepsy and IH. Jazz Pharmaceuticals plans to apply to have its drug Xywav approved by the FDA for IH in 2021, which could make Xywav the first ever approved for the IH indication.
The neurochemical mechanisms behind IH remain largely mysterious. The Emory work on patients’ response to flumazenil suggested that substances resembling benzodiazepines were weighing down the brain. It’s an appealing idea; if an antidote to a drug wakes somebody up, then something similar to that drug was making them sleepy. The notion that the brain might contain endogenous benzodiazepines or “endozepines” stretches back to the 1970s, when scientists were figuring out how the drugs worked.
When Rye was trying to publish his team’s results a decade ago, his peers around the world were skeptical. The 1997 incidents in Tuscany had discredited the mechanism he was proposing. If someone wakes up with flumazenil, that person was probably on benzodiazepines, and the burden is on you to prove otherwise, Rye was told. His team’s findings were eventually published, although they are still disputed today.
Rye, a formidable physician-scientist who is an important part of my book, has called the idiopathic recurring stupor story “fake news.” So why explore it two decades later? I wanted to figure out whether something produced within the human body could act like a benzodiazepine — and what that substance might be. Also, in discussions with sleep researchers, I learned that some people didn’t know what actually happened. The story illustrates the limitations of forensic science and the distortions of media coverage. We have to see how things can go wrong to know how to put them right.
The lethargics
During the first episodes of sudden sleepiness in 1997, the woman in her 80s was taken to a hospital in Lucca. Tests such as brain MRI, electrocardiogram and toxicology did not explain what had happened. Then the weird somnolence started to hit others. One woman was folding laundry on her balcony, when she felt her head becoming heavy. She lost her balance and her husband had to help her inside. The first patient’s daughter lived a few kilometers away, but she was struck when she was driving back from visiting her mother. Her car ran into a wall, causing minor injuries. By the end of August, a doctor named Attilio Favilla, who had cared for the sudden sleepers, became alarmed and asked the local health department (Unita Sanitaria Locale or USL) for help.
Domenico Tani, then an enterprising reporter for regional newspaper Il Tirreno, published the first story on the phenomenon in September.
“If you only talk to the police and the officials, you only get the official stories,” he recalled. “You need to go to the bars and cafes and talk to the regular people.”
At first, newspapers did not print affected individuals’ full names. They were described collectively as the “lethargics” (letargici). By September 24, Camigliano residents were complaining to Tani that they were under siege from crowds of reporters, and that a television crew had barged into someone’s house. Newspapers had fun speculating about what was going on. Corriere della Sera interviewed UFO enthusiasts. La Nazione investigated whether soporific radon gas was emerging from the earth. La Stampa warned: “The virus of lethargy infects Lucca”. The UK’s Times joined in with: “Drowsy Tuscan town roused by epidemic of ‘sleeping sickness’.” (Note: I’ve used Google Translate on links to the Il Tirreno archives, which are available online.)
To be clear, nobody in Lucca itself was affected. Camigliano lies nestled in the hills, about 10 kilometers east of Lucca and its centuries-old grass-topped walls. The investigation centered on a few houses around a courtyard garden, a pleasant spot decorated with begonias and geraniums where a group of neighbors socialized. Public health officials first looked for an environmental cause, testing water wells and quizzing residents about their eating habits. They inspected the paint and carpet in residents’ homes and the gas lines in their kitchens. Suspicion fell upon a mobile telephone tower that had recently begun operation. An environmental advocacy group demanded the shutdown of nearby high-voltage electric lines. Nothing emerged that could account for the “sleeping sickness.”
All the media attention brought an intervention. Giuseppe Plazzi, a neurologist from the University of Bologna, arrived in the second half of September. Lugaresi had charged Plazzi with evaluating the sudden sleep phenomena and assisting the USL investigators. Plazzi had been on vacation with his family when Lugaresi called, telling him to buy a newspaper to catch up and then go to Tuscany. When talking with me two decades later, Plazzi, now one of the world’s top experts on narcolepsy, showed affection for his former boss, but also shook his head at the events that followed that call.

Annoyed about ending his vacation, Plazzi followed orders, bringing along a colleague, pharmacologist Roberto Riva. When they showed up, a television crew was already interviewing Camigliano residents. They were eager to have the doctors examine them, Plazzi recalled in an interview. Fortuitously, a 51-year old woman fell into a lethargic state while the doctors were there.
In the account in Plazzi’s book The Three Brothers Who Never Slept, he wrote that the woman lay on a couch “motionless, as if her eyes had crossed the eyes of Medusa.” She was breathing regularly, but didn’t respond to shaking. The woman was taken to a Lucca hospital, where Plazzi was able to survey the EEG patterns made by her brain while she was asleep. He detected a characteristic high frequency pattern suggesting that she was under the influence of benzodiazepines. Plazzi and Riva gave her flumazenil, which quickly woke her up. The Bologna doctors instructed their Lucca colleagues on how to provide the same treatment on their own and took blood samples for additional investigation.
Favilla and local pharmacists confirmed affected individuals’ assertions that they had not taken sleeping pills. When blood samples from Camigliano were analyzed in Bologna, Lugaresi announced a tentative diagnosis: idiopathic recurring stupor.
Charming and persuasive
Lugaresi and his colleagues had already published several papers on IRS. What was distinctive about the Camigliano cases was that they came in a cluster. Previously, they were scattered, occurring one at a time. Their 1994 paper in Neurology contains a description of one case, provided by a patient’s wife:
“He talks and walks like a drunk, looks drowsy, but insists he feels well. He wants to leave his house and becomes aggressive if somebody tries to stop him. He had several car accidents in this condition. Drowsiness progresses to a deep sleep with snoring, lasting 8 to 12 hours. He can be awakened with vigorous stimuli, but he soon goes back to sleep. He gets up to eat, still groggy and confused, and then goes back to sleep. This condition usually lasts for 3 days until he recovers completely and remembers nothing about what happened.”
The Bologna neurologists reported being unable to detect alcohol or benzodiazepines in the man’s body. That was odd, because his EEG patterns looked like those of someone on benzodiazepines. When the doctors gave him intravenous flumazenil, he woke up and was alert — but only for 40 minutes. He had been experiencing stuporous episodes every few weeks for two years. When he wasn’t having an episode, he didn’t doze off quickly in the sleep lab, so he didn’t have IH or narcolepsy. The man and two others came from different regions of Italy, so an artificial, external cause was thought unlikely. The three “were disturbed by their episodes and irritated at being suspected of being alcoholics.”
Because of Lugaresi’s prominence, his pronouncements carried some weight. He had organized an early international meeting of sleep scientists, held in Bologna in 1967, and he was one of the first to notice sleep apnea’s effects on blood pressure. One of his foremost contributions to neurology and sleep medicine was the characterization of fatal familial insomnia (FFI), a rare inherited neurodegenerative disease. As the name suggests, the disease begins with insomnia, progresses to hallucinations, panic attacks and eventually, dementia and death.

In the 1980s and 1990s, Lugaresi and his team in Bologna, together with Pierluigi Gambetti at Case Western Reserve, defined FFI and discovered the gene responsible. It is caused by a mutation altering the same prion protein that misbehaves in mad cow disease, scrapie (affecting sheep), and Creutzfeldt-Jakob disease in humans. The prion clumps destroy the thalamus, a region of the brain that is a gatekeeper for sensory signals.
Lugaresi, who died in 2015, appeared in The Family that Couldn’t Sleep, New Yorker writer D.T. Max’s book on prions and fatal familial insomnia. Max described Lugaresi as “charming and persuasive” and as a lover of fine foods and wines. He wrote: “Lugaresi liked his work and was good at it, becoming known internationally for his subtle reading of the EEG printouts his sleep lab produced and, within Italy, for his ability to shake loose funding from the bureaucracy.”
On IRS, Lugaresi had been collaborating with Jeffrey Rothstein, a young neuroscientist from Johns Hopkins. As part of his research on alterations of brain chemistry during liver failure, Rothstein had refined methods for separating benzodiazepine-like chemicals. He had assisted the Bologna researchers with analyzing some of the IRS samples, although not those from Camigliano.
Using Rothstein’s methods, the Bologna researchers could process a sample of blood or spinal fluid, put it into a chromatography instrument, and peaks would appear on a graph. The chromatography analysis showed that endozepines behaved similarly to synthetic benzodiazepines: they were the same molecular size. But it couldn’t show exactly what the peaks represented.
My book delves into why the idea of endozepines was so captivating to pharmacologists and neuroscientists. They satisfied the conceptual need for a natural counterpart to Valium, and they also helped to explain the surprising effects of flumazenil, which was supposed to be an inert antagonist that displaced benzodiazepines from their binding sites.
When considering Lugaresi’s interest in endozepines, we can note that he was good friends with Giuseppe Scollo-Lavizzari, the first neurologist to use flumazenil as an antidote in an emergency room setting. Scollo-Lavizzari had tested flumazenil on patients with liver failure, and Lugaresi’s team had previously tried the drug on an FFI patient. For Lugaresi, the idea that flumazenil could bring someone out of an altered mental state wasn’t strange, even if the person wasn’t on benzodiazepines.
Where endozepines came from, and what they actually consisted of, were not clear. The term has sometimes been used for a protein named diazepam binding inhibitor, but Lugaresi’s group thought they were seeing something else: smaller drug-like molecules. Human cells are not known to produce chemicals that have a benzodiazepine-like chemical structure, but bacteria, molds and fungi can. Maybe small amounts of these substances in foods were being converted within the body into something more potent. Whatever their origin, when Lugaresi’s team looked at the samples from Tuscany, they spotted “endozepine 4,” which they had seen before in their IRS patients. Lugaresi told reporters: “We are 99 percent sure that the substance found in this first analysis is also present in the blood of the other eight people in Lucca.”
Animals in a cage
Lugaresi’s announcement spurred more environmental fact-finding, and more speculation. In Camigliano, outside the homes of the lethargics, the USL set up a mobile laboratory for monitoring air quality. One proposal, pursued by public health officials, was that sleepers’ bodies were metabolizing pesticides from a nearby farm into endozepines. Plazzi said a local hunter offered him carcasses of birds to test for suspicious chemicals.
Sudden sleep incidents continued in September and October. Camigliano hosted television crews from Italian national broadcaster Rai, Germany and the UK. Residents reported feeling frustrated and “like animals in a cage, reduced to guinea pigs.” Newspapers interviewed the youngest of the lethargics, who said the experience of being woken by flumazenil three times during one hospital visit was not pleasant, because its effects arrived and wore off quickly. She said if the lethargy hit her again, she should not be taken to the hospital but simply left at home. A few days later, a mother and son, both of whom had been hit by sudden sleep before, fell asleep together at the kitchen table.
At the end of October, the USL declared its intention to evacuate the lethargics from their homes for a few months. The goal was to test if the cause of the incidents was environmental. The idea came from the Lucca public prosecutor’s office, which told news organizations its interest was based on possible environmental pollution. At the beginning of November, several residents cleared out of their houses and went to stay with friends or relatives, saying they felt “like earthquake victims.”
Meanwhile, Lugaresi’s team in Bologna made a transition to better tests. They figured out that “endozepine 4” in samples from Camigliano’s sudden sleepers was in fact lorazepam, a widely available anti-anxiety and insomnia drug. Known commercially as Tavor in Italy or Ativan in the United States, lorazepam is more potent than diazepam/Valium, and is eliminated from the body more quickly. The key to seeing it was mass spectrometry, which allows scientists to break apart a chemical to see what it’s made of, even if tiny amounts are available.
On October 24, Lugaresi sent a letter to the USL informing them that in samples from the sudden sleep cases, lorazepam had been positively identified. The result was not discussed openly until two weeks later, when Lugaresi and the USL broke the news together. There was no need to hunt for the cause of an exotic new disease. Instead, prosecutors proposed, a sneaky person may have introduced the drug into sudden sleepers’ food or drinks.
When interviewed by La Nazione, Lugaresi deferred to others on questions of criminality: “I can only say that, by exampling the blood samples of the seven people of Lucca, traces of benzodiazepines, substances present in sleeping pills and anxiolytics, have been found in all of them. Now the investigation will be continued by the leaders of the USL and authorities in Tuscany.”
Camigliano residents were shocked and afraid. Attilio Favilla, the doctor who had set the ball rolling that summer, reiterated that he had not prescribed Tavor to affected individuals. Investigators reviewed more than 30 sudden sleep incidents, trying to determine whether someone had a chance to act covertly. In retrospect, some looked suspicious, such as the time a woman fell into lethargy after returning from having coffee with friends. But others seemed impossible; on another day, the same woman went into somnolence just after taking a shower, before breakfast.
By the middle of November, charges were announced against a married couple who were neighbors of some of the lethargics. In a twist, the female suspect had been hit by the lethargy herself — and newspapers had interviewed her about it. She had looked after the initial elderly victim, cooking and performing other household tasks for her. Her husband, a paper mill worker on disability, allegedly had provided lorazepam from his own supply. In a meeting with Il Tirreno reporter Domenico Tani, prosecutors asked whether Tani had colluded with the female suspect and had an affair with her, suggestions he found preposterous.
Although it appeared that no physical harm had come to the sudden sleepers, they could have had more serious car accidents, choked on food, or fallen down stairs. A fatal overdose of lorazepam is difficult to achieve by itself, but is more likely if the drug is combined with alcohol, or given to someone with existing cardiac or respiratory troubles. Several of the lethargics were in their 70s or 80s. An Il Tirreno headline summarized their reaction: “Anger and dismay after seven months of hell.”
Heat and light
Before the trial in Lucca began in 1999, three scientific communications told the Bologna side of the story. A January 1998 paper in Brain collected information on 20 cases of idiopathic recurring stupor, not including the Camigliano lethargics. The authors proposed that IRS be renamed “endozepine stupor,” citing the links between the symptoms, the presence of endozepine 4 and the effects of flumazenil.

The Brain paper was submitted at the end of 1996 and accepted in August 1997, just before the Camigliano incidents began to appear in the news. A map from the paper showed IRS cases distributed around Italy, and the paper refers to other reported cases in South Africa and Canada. The clinical details were similar to what Lugaresi’s team had published previously. Some patients progressed from a stupor into a temporary coma, and they could not be woken by physical stimuli. The researchers used a form of mass spectrometry that might have shown endozepine 4 was lorazepam, but they did not detect the overlap. In light of the charges against the Camigliano suspects, some interpretations in the Brain paper read uncomfortably:
“In some cases, intentional intoxication by relatives had been covertly suggested by the treating physicians, with disastrous consequences on family life. A correct early diagnosis of endozepine stupor is therefore mandatory.”
In a follow-up letter a few months later, Lugaresi, Plazzi and colleagues reported they had found lorazepam in the Camigliano samples using a more sensitive set up: liquid chromatography-mass spectrometry. They concluded that an endozepine origin for other IRS cases “should be considered as still unproven.” The 1998 paper was not explicitly labeled as retracted, leaving a confusing record for other scientists to follow.
A second exchange in The Lancet added more heat than light. Prompted by a teasing letter from an anesthesiologist in Lucca, the Bologna doctors claimed that they had always been suspicious of the Camigliano IRS cases:
“…despite the negative toxicological findings our instinct told us to look out for benzodiazepine overdose, so we carried on sniffing around for these, as well as the endozepines, in the patients’ plasma samples. We finally managed to identify lorazepam…Naturally, we informed the magistrate, but otherwise we kept our findings strictly to ourselves, to avoid hampering early legal investigations, which subsequently led to the offenders — who appeared to have been poisoning their neighbours — being accused.”
In contrast, when Lugaresi announced that lorazepam was a likely cause of the sudden sleep incidents, he undercut an ongoing criminal investigation, Plazzi said. Prosecutors were unhappy with Lugaresi’s haste, because it may have driven suspects to destroy evidence. Some support for this did emerge at trial. A neighbor had spotted the suspects at night at their homes, after they had already evacuated. This led the neighbor to accuse them of removing medicine bottles in a suitcase. A search by police afterwards was unproductive. Still, prosecutors had not been shy about questioning Camigliano residents, so suspects were probably on guard already.
Evidence presented against the accused at trial was circumstantial, according to both newspaper accounts and a later review at the University of Bologna (kindly provided by Francesca Ingravallo). Nobody ever saw the suspects introduce pills or drops into the victims’ food or drink, and it wasn’t clear that anything had been taken from the victims during their impaired states. One of the victims told prosecutors she once noticed “strange bubbles” on the surface of a dish of soup prepared by her neighbor. This testimony is questionable, because of the disruptive effects of lorazepam on memory. The case against the female suspect was mainly that she was present at the right times, and her husband was supposed to have supplied the drugs. Prosecutors speculated that she may have been motivated initially by spontaneous gifts from the victims, by the opportunity to receive attention, and later, expenses paid for television appearances.
In court, controversy arose over how much lorazepam was necessary to put someone to sleep, with pharmacologist Riva testifying that 10 mg would produce a lethargic effect in young healthy people, and that half as much would have been sufficient in elderly people.
“The defense therefore argued that in order to continuously subjugate the subjects, it would be necessary to have several different vials of medication available and that they should have been found in the garbage or somewhere else,” Riva recalled in an email. “I still believe that the subjects were periodically intoxicated by someone. Over time, we had several other experiences of this type, always with lorazepam.”
Why wasn’t lorazepam identified in the Camigliano cases sooner? No emergency room in Italy could have detected its presence, Plazzi told the court. Normal toxicology tests, based on commercially available antibody-based assays, were not sensitive enough, especially for lorazepam. Even mass spectrometry was tricky.
In 1999, the accused couple was acquitted in Lucca. In the Italian justice system, in contrast to the United States, prosecutors have the option of appeal. They were able to convict two years later. According to Il Tirreno, the female suspect lost her job and had to move in with her daughter. In 2002, the case reached the Italian Supreme Court, which cited the lack of hard evidence and threw it back, leading to the female suspect’s exoneration in 2003. Among her former neighbors, bitterness remained.
Seduced by an exotic diagnosis
After the Camigliano cases unraveled, idiopathic recurring stupor had an uncertain status. In 2003, neurologists from Australia warned other clinicians to beware of IRS, based on experiences with an elderly male patient, who had a 16 year history of recurrent stupor and coma episodes. They initially diagnosed him with IRS, even though urine tests suggested otherwise. The patient’s wife, who had a history of benzodiazepine dependence, eventually confessed to giving the drugs to both her husband and her mother.
The Australian neurologists surmised that they had observed Munchausen syndrome by proxy, in which caregivers invent, induce or exaggerate physical or psychological symptoms in others. Munchausen syndrome by proxy had usually been reported with a mother as perpetrator and children as victims, but “a pleasant elderly country gentleman, always accompanied by his appropriately worried wife, gave no reason for us to suspect drug abuse.” The doctors had been “seduced” by the exotic diagnosis of IRS instead.
The Australians challenged the Bologna group, asking whether endozepine stupor was a viable concept. Sneaky benzodiazepine administration was responsible for some cases — what was really happening with the others? Munchausen syndrome by proxy is a better explanation, they wrote.
At the time, Lugaresi and his colleagues were retracing their steps, analyzing samples from their previous cases. One man who had been diagnosed with IRS sued the University of Bologna when when informed of the revised findings. He had experienced stuporous episodes while on vacation in Sardinia and at home. A domestic helper with access to lorazepam may have been responsible; once that person moved away, the episodes stopped.
Over the years, the Bologna team has been able to clear up most of the IRS incidents. Riva told me: “The issue is delicate. In some of these cases, we also identified those who periodically poisoned the subjects and why. In almost all cases, there was admission of responsibility. As the perpetrators were close relatives, the issues resolved without the intervention of the judiciary, and the episodes have not reappeared.”
Not all putative IRS cases have resolved gracefully. In 2015, separate from the Bologna group, neurologists from the University of Sassari reported a case that looked like idiopathic recurring stupor. A 76-year-old man was brought unconscious to the emergency department several times. Although benzodiazepines were not detected, he was revivable with flumazenil. The man’s story ends on a tragic note:
“Although some peculiar features in the family history pointed to a possible Munchausen syndrome by proxy, no concrete evidence came out even after the patient and his family had been questioned different times. The patient became more and more frustrated by the condition which we could not explain or stop, and he died after committing suicide.”
Currently, idiopathic recurring stupor appears to have been a mirage. In a 2014 paper published in Sleep, members of the Bologna group confirmed that samples from their IRS cases contained synthetic benzodiazepines. They concluded: “Spontaneous IRS is therefore an unproven and indeed questionable entity.” When talking with me, Plazzi was blunter, saying: “Idiopathic recurring stupor does not exist.”
Forensic techniques have now advanced enough so that benzodiazepines can be detected in hair samples, which could have been useful back in Camigliano/Lucca. Unlike urine or blood tests that can only detect drug use within the last few days, hair analysis can detect use months ago. Even so, lorazepam is harder to detect than other drugs of abuse. It was not until 2010 that forensic scientists reported the ability to detect a single dose of lorazepam from a hair sample. Plazzi was co-author on a 2018 paper using hair analysis to detect benzodiazepines in a suspected case of recurrent stupor.
University of Bologna medical student Laura Zangheri eventually wrote her thesis on IRS. Zangheri suggested that Lugaresi’s team was swayed by error of preconception, or confirmation bias. That is, they focused their attention on endozepines because that’s what they were interested in already. Zangheri cited 19th century Italian medical scholar Augusto Murri, who wrote that doctors had a tendency to chase the “unknown fantasy”, rather than the “marvelous truth.”
The fish that got away
After learning about what had happened in Italy, I wanted to find out what other researchers thought about the endozepine episode. So I turned to Jeffrey Rothstein, the neuroscientist at Johns Hopkins who had helped Lugaresi analyze IRS samples. At the start of his research career, Rothstein was looking for benzodiazepine-like substances in animal brains. He was commuting back and forth to Washington DC, pursuing work on ALS (amyotrophic lateral sclerosis) at Hopkins at the same time.
In a 2018 interview at his office, Rothstein showed me old printouts and graphs from his experiments. He had obtained hundreds of pounds of cow brains and extracted them with organic solvents such as chloroform. In one of his papers, he hinted that he had isolated something from cow brains, and knew the molecular weight, but not the precise structure. He also tried using fungi as raw material, which smelled awful, he said.
In his later career, Rothstein turned away from research on endozepines. Instead, he became an authority on ALS. But he never stopped thinking that the brain contains benzodiazepine-like compounds. After all, it was unlikely that anyone was sneaking around giving cows lorazepam, he said.
“I truly believe that something is in there,” he said. “I just gave up looking for it.”
Thanks to Giuseppe Plazzi, Francesca Ingravallo, Domenico Tani and Jeffrey Rothstein